Hydrostatic Pressure does not cause detectable changes to Survival in Human Retinal Ganglion Cells
Osborne, Andrew . 2015
PURPOSE:
Elevated intraocular pressure (IOP) is a major risk factor for glaucoma. One consequence of raised IOP is that ocular tissues are subjected to increased hydrostatic pressure (HP). The effect of raised HP on stress pathway signaling and retinal ganglion cell (RGC) survival in the human retina was investigated.
METHODS:
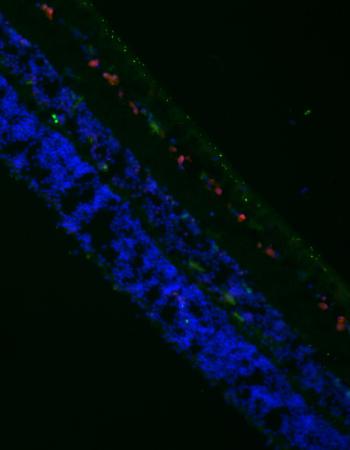
A chamber was designed to expose cells to increased HP (constant and fluctuating). Accurate pressure control (10-100 mmHg) was achieved using mass flow controllers. Human organotypic retinal cultures (HORCs) from donor eyes (<24 h post mortem) were cultured in serum-free DMEM/HamF12. Increased HP was compared to simulated ischemia (oxygen glucose deprivation, OGD). Cell death and apoptosis were measured by LDH and TUNEL assays, RGC marker expression by qRT-PCR (THY-1) and RGC number by immunohistochemistry (NeuN). Activated p38 and JNK were detected by Western blot.
RESULTS:
Exposure of HORCs to constant (60 mmHg) or fluctuating (10-100 mmHg; 1 cycle/min) pressure for 24 or 48 h caused no loss of structural integrity, LDH release, decrease in RGC marker expression (THY-1) or loss of RGCs compared with controls. In addition, there was no increase in TUNEL-positive NeuN-labelled cells at either time-point indicating no increase in apoptosis of RGCs. OGD increased apoptosis, reduced RGC marker expression and RGC number and caused elevated LDH release at 24 h. p38 and JNK phosphorylation remained unchanged in HORCs exposed to fluctuating pressure (10-100 mmHg; 1 cycle/min) for 15, 30, 60 and 90 min durations, whereas OGD (3 h) increased activation of p38 and JNK, remaining elevated for 90 min post-OGD.
CONCLUSIONS:
Directly applied HP had no detectable impact on RGC survival and stress-signalling in HORCs. Simulated ischemia, however, activated stress pathways and caused RGC death. These results show that direct HP does not cause degeneration of RGCs in the ex vivo human retina.

PURPOSE:

Education in the ethical conduct of research that is acquired by postgraduate students is a key component
for their professional development in scientifi c and academic communities. This…

This study compared efficacy of two polyvalent antivenoms (Saudi Arabian and Egyptian), against lethality and pathophysiological changes of …